New peer-reviewed clinical research unpicks the relationship between oral bacterial imbalances and the development of oral cancers. It highlighting the importance of maintaining a balanced microbial health for helping to prevent oral cancers, and providing some insights into how these can be identified and treated by dental professionals in the future.
It is known that an imbalance between microbes can increase the risk of numerous diseases including cancer in humans. Oral microbiota plays a role in the human microbiome and thereby human health, and chronic inflammation and systemic diseases can be the result of microbial imbalances, contributing to the development of cancerous cells.
As a proportion of all cancers in humans, head and neck cancers account for 5%, of which half occur in the oral cavity. Since the 1990s researchers have examined the link between bacteria and carcinogenicity in various organs in the human body. The more recent emergence of next-generation sequencing (NGS), 16S rDNA sequencing has assisted this vein of inquiry, making insights into potential diagnostics and identifying specific bacteria as being associated with development of OSCC.
Oral squamous cell carcinoma (OSCC) is a type of head and neck cancer, and it makes up 90% of all oral cancers, with an increasing incidence in Australia and worldwide. Even with advances in radiotherapy, chemotherapy and surgical methods, the survival rate is in the region of 50-60%.
The key lifestyle risk factors for OSCC include smoking, alcohol consumption and chewing betel, with viral infection, fungal infection and chronic periodontitis also identified.
Researchers set out to determine the characteristics of the relationship between oral microflora and OSCC, as well as how the multitude of certain bacteria could be used as a biomarker to predict OSCC with high diagnostic accuracy.
The study compared the microbiota compositions between tumour sites with normal tissue samples in buccal mucosal of 50 patients with OSCC, as well as with a control group consisting of samples from healthy individuals, using 16S rDNA sequencing.
A significant difference in the oral bacterial profiles was found, where cancerous cells were shown to have both more numerous, and a wider range of bacteria types, compared with the healthy tissue samples. Elevated levels of Fusobacterium nucleatum, Prevotella intermedia, Aggregatibacter segnis, Capnocytophaga leadbetteri, Peptostreptococcus stomatis, plus five other species were found, indicating a potential association between these bacteria and OSCC. In particular, F.nucleatum was found to be the most prevalent, showing virulence factors in the tumor sites. It is already known that F.nucleatum is linked with human colorectal carcinoma via immune suppression.
The diagram summarises the research findings regarding the species of bacteria, their role in oral health, and the pathogenic cycle the results from disequilibrium in oral microbiota. As the volume and range of healthy bacterial species (identified in red text) reduces, the oral microbiota equilibrium is disrupted. The increase in the prevalence of three main bacterial species (identified in blue text) is identified, together with the ensuing pathogenic cycle, which results in the triggering and then progression of oral cancer.
In addition, genes associated with pathological processes were markedly higher in the OSCC group, aiding cancer-causing inflammation. Whilst acute inflammation is thought to be a part of the body’s immune system, chronic inflammation can lead to cancerous growth.
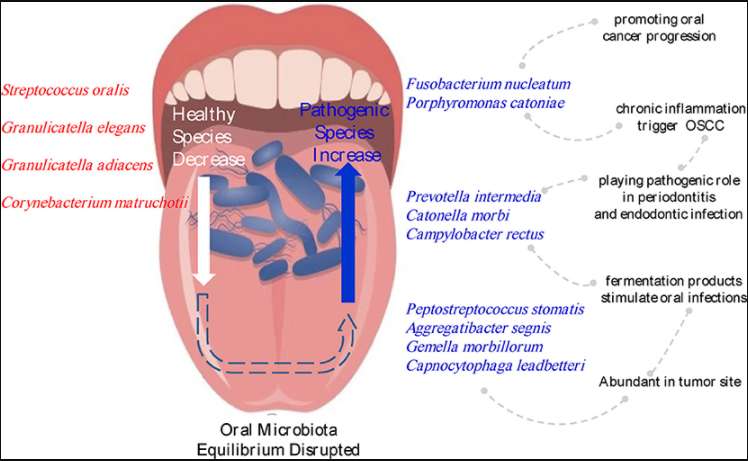
Image – Changes in the microbiota composition associated with OSCC
The study concludes by suggesting that reintroducing a more balanced bacterial composition may interrupt the action of the pathogenic bacterial increase. These findings could be a source of diagnostic markers, therapies and treatments for oral cancer and recommends further research into these suggestions.
Research and image Citation: Zhang L, Liu Y, Zheng HJ and Zhang CP (2020) The Oral Microbiota May Have Influence on Oral Cancer. Front. Cell. Infect. Microbiol. 9:476. doi: 10.3389/fcimb.2019.00476. As published in www.frontiersin.org
We are always keen to improve our information for the dental community. If you have an idea for a blog post, we would be happy to hear from you.
Contact us today on 1800 118 991 or editor@thedentalreview.com.au
PO Box 2345, Parramatta NSW 1750 Australia
T: 1800 118 991
E: editor@thedentalreview.com.au