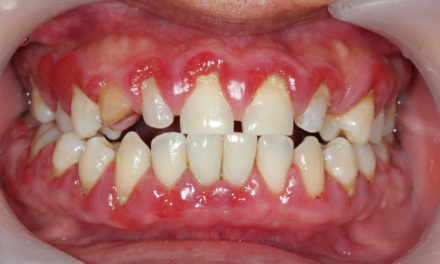
How often does a dentist start to tackle a tooth – maybe cracked, but otherwise intact and needs to take a PA xray? But then the patient gags!
Foul thoughts abound and repeated efforts often just make things worse. But maybe it’s time to understand a little more about this important reflex and what it is signalling.
What is gagging? It’s an oral airway protective reflexive response. So why is this important?
The short answer is that it’s signalling the brain’s displeasure of having already lost the ability to nose breathe the impending loss of the oral airway is alarming and it puts measures in place to rectify this situation.
This poses a deeper question – that of what does it mean for a dentist. The answer is often subtle and complex, as all things can be, but as a simple person, I look at life as simply as possible. Simply – if you don’t breathe you die! Then there are all the in-between ranges of airway impairment and the degrees of oxygen saturation. For example where the levels drop slightly in the brain and then recover (Dipping) there is remarkably high adverse inflammatory reaction seemingly out of proportion to the change. But there is less response where the person simply stops breathing for half a minute with greater drop in brain oxygen. Gozal (1) showed the exhaled breath of non-obese snoring 3 year olds has about as many inflammatory chemicals as an adult who recently had a cardiac whereas those who did not snore were near-clean. As most pathology involves inflammation this is a biggie.
How does all this relate to gagging you ask – well hopefully you do ask.
My reading and research of hundreds of cases shows that the underlying cause/s are linked to societal changes. These rose sharply in the second half of the 19th Century and seem to have peaked in the late 20th Century. The increase in sugar consumption and in tobacco with their commercialisation in the Caribbean and Southern USA at the turn of the 19th C. UK sugar levels rose from Shakespeare’s time at around 1lb (500 grams) and seems to have plateaued or peaked in the mid 1990’s at over 200lbs. Sugar is involved in most consumables – even toothpaste. Sugar appears with three ‘friends’ that act epigenetically by inducing HOX genes that in turn dampen the actions of neural crest cells – the fringes of the embryological foetus before the neural plate curls into the neural tube. French and Belgium teams in the 1990’s showed that these factors (sugar – smoking- alcohol and probably maternal sleep fragmentation) combine to impair the midface growth leading to a narrow and ‘shortened’ naso-maxilla. (2-7). This was first signalled in the dental context by Harvold (8-13) as an entity when he blocked one nostril in infant monkeys and induced asymmetrical growth. Equally the lower jaw is generally less impacted with resulting mandibular entrapment and being forced backwards, carrying the tongue into the throat.
These combined mean the nose is frequently out of action and this is noted in some general medicine with people such as Prof Dr. Christian Guilleminault and his request that all dentists ensure 100% nasal breathing – Prof Dr. Giles Lavigne who warns that stopping the dental effects of bruxing with a night-guard may exacerbate the very cause, which is the same as gagging – that is alterations in breathing patterns with gas-levels changing leading to arousal and then parafunction. It is well recognised that Bruxism is preceded by an arousal as seen in sleep studies. (14-19) Lavigne warns the bulk of a night-guard can take away some if not most of the oral airway (20). Many night guards live in the bathroom or found in the bed on waking. So the actions of airway protection are those of the brain protecting its oxygen supply, but equally important is that this is just one aspect of the oral manifestations of a compromised midface growth and impairment of the airways. Gagging, bruxing and sleep apnoea as well as TMJ problems are inextricably entwined.
For those who like lists, this is mine of oral signs starting at the lips.
- Lips apart – mouth breathing (important as it draws dry cold dirty air over tonsils and into the lungs and takes out up to six times more carbon dioxide than nose breathing thereby upsetting both pH of blood and of biochemistry as seen in metabolic changes – Type two diabetes is five times more prevalent in ‘snorers’ or more accurately OSA/SDB.
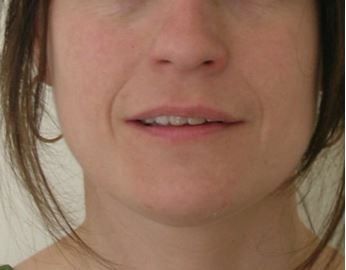
- Worn incisors. Secondary to mandibular protrusion, which opens the throat and pharyngeal airway, but not adequately in many and there is still bruxing.
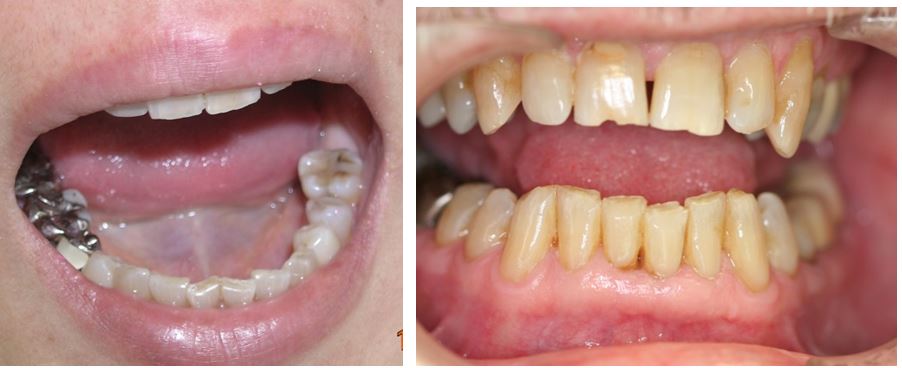
These are typical of incisal wear, often some are far worse than these. Also Buccal ‘erosions’ – arguably abfractions.
- Tongue scalloping Lateral borders with indentations of the teeth indicating life-long inadequate tongue space where if there isn’t enough oral space the tongue compromising the pharynx.
- Cheek biting. A line or ‘ridge’ along the level of the teeth. Often seen in patients and indicates buccinators activity- again secondary to a poor airway.
- Tongue resting on top of lower teeth.
- No visible airway. This is most commonly scored 0-4 in the Mallampati Score – a measure developed by an anaesthetist.
- Erosion linked to GERD is a reasonable addition as reflux is slightly higher prevalence in Sleep Apnoea, (38% vs 32%) but few studies consider the estimated 9% of juveniles with silent reflux. The most common sign are the cup-like craters on the tips of lower molars. (21-23)
A lot of these manifestations are visible on lateral head xrays including the level of the Hyoid bone and the AP dimension of the throat – above the Glottis.
I also look at the curve of the neck – which should be smooth, but often isn’t. Narrow these airways may be all these patients were awake and compensating. Frequently pharyngometery reveals during sleep these probably halve. These kids will all hate impressions.
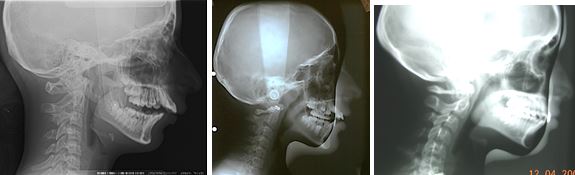
Three very different lordotic curves and associated pharyngeal profiles.
A good clue to the core problem of sleep disruption can be hyperactivity in children and Dr. K Bonuck points to this (24-27) as do (28-30) Antonio (Bruxing in children- a warning sign for psychological problems?) Delgado (Bruxism a warning sign) Manfredini & Lobbezoo, very well accepted researchers on current concepts in bruxism. Gagging is often a clue to these patient profiles.
So when your patient gags, perhaps think more of sympathy and check their medical history and medications. A great number of them will have such as reflux – with ‘Losec’ to subdue it and antihypertensives, antidepressants and sleeping tablets, as well as other medications.
A glimpse at their medications can be revealing and a good guide to longevity of restorative work, and via systemic inflammatory processes integrity of bone both regards perio and of course implants.
Maybe you could consider viewing or reviewing the role of the dentist and think of including the airway as part of your daily thought patterns. We all have them and more than half show the results of impairment. Perhaps start with taking impressions in an sitting upright position.
It’s a great new and important field of everyday dentistry.
Dr. David Zimmerman BDS Post Grad Cert Pain and Pain Management.
- Gozal. Metabolic alterations and systemic inflammation in OAS among non-obese and obese prepubertal children. Am Jnl Resp and Crit Care [Internet]. 2008; 177:[1142-9 pp.].
- Borday C, Wrobel L, Fortin G, Champagnat J, Thaëron-Antôno C, Thoby-Brisson M. Developmental gene control of brainstem function: views from the embryo. Prog Biophys Mol Biol. 2004;84(2-3):89-106.
- Creuzet S, Schuler B, Couly G, Le Douarin NM. Reciprocal relationships between Fgf8 and neural crest cells in facial and forebrain development. Proc Natl Acad Sci U S A. 2004;101(14):4843-7.
- Le Douarin NM, Creuzet S, Couly G, Dupin E. Neural crest cell plasticity and its limits. Development. 2004;131(19):4637-50.
- Le Douarin NM, Couly G, Creuzet SE. The neural crest is a powerful regulator of pre-otic brain development. Dev Biol. 2012;366(1):74-82.
- Helms JA, Kim CH, Hu D, Minkoff R, Thaller C, Eichele G. Sonic hedgehog participates in craniofacial morphogenesis and is down-regulated by teratogenic doses of retinoic acid. Dev Biol. 1997;187(1):25-35.
- Sperber GH. Current concepts in embryonic craniofacial development. Crit Rev Oral Biol Med. 1992;4(1):67-72.
- Anderson G, Fields HW, Beck M, Chacon G, Vig KW. Development of cephalometric norms using a unified facial and dental approach. Angle Orthod. 2006;76(4):612-8.
- Ball JV, Hunt NP. Vertical skeletal change associated with Andresen, Harvold, and Begg treatment. Eur J Orthod. 1991;13(1):47-52.
- Harvold EP, Tomer BS, Vargervik K, Chierici G. Primate experiments on oral respiration. Am J Orthod. 1981;79(4):359-72.
- McNamara CM. A retrospective cephalometric study of the effects of the Harvold appliance in the treatment of 20 patients with a Class II division 1 malocclusion. J Ir Dent Assoc. 1989;35(1):36-8.
- Tomer BS, Harvold EP. Primate experiments on mandibular growth direction. Am J Orthod. 1982;82(2):114-9.
- Woodside DG, Altuna G, Harvold E, Herbert M, Metaxas A. Primate experiments in malocclusion and bone induction. Am J Orthod. 1983;83(6):460-8.
- Aguglia U, Gambardella A, Quattrone A. Sleep-induced masticatory myoclonus: a rare parasomnia associated with insomnia. Sleep. 1991;14(1):80-2.
- Carra MC, Rompré PH, Kato T, Parrino L, Terzano MG, Lavigne GJ, et al. Sleep bruxism and sleep arousal: an experimental challenge to assess the role of cyclic alternating pattern. J Oral Rehabil. 2011;38(9):635-42.
- Herrera M, Valencia I, Grant M, Metroka D, Chialastri A, Kothare SV. Bruxism in children: effect on sleep architecture and daytime cognitive performance and behavior. Sleep. 2006;29(9):1143-8.
- Huynh N, Kato T, Rompré PH, Okura K, Saber M, Lanfranchi PA, et al. Sleep bruxism is associated to micro-arousals and an increase in cardiac sympathetic activity. J Sleep Res. 2006;15(3):339-46.
- Itani O, Kaneita Y, Ikeda M, Kondo S, Yamamoto R, Osaki Y, et al. Disorders of arousal and sleep-related bruxism among Japanese adolescents: a nationwide representative survey. Sleep Med. 2013;14(6):532-41.
- Kato T, Masuda Y, Yoshida A, Morimoto T. Masseter EMG activity during sleep and sleep bruxism. Arch Ital Biol. 2011;149(4):478-91.
- Gagnon Y, Mayer P, Morisson F, Rompré PH, Lavigne GJ. Aggravation of respiratory disturbances by the use of an occlusal splint in apneic patients: a pilot study. Int J Prosthodont. 2004;17(4):447-53.
- Alfaro EV, Aps JK, Martens LC. Oral implications in children with gastroesophageal reflux disease. Curr Opin Pediatr. 2008;20(5):576-83.
- Linnett V, Seow WK. Dental erosion in children: a literature review. Pediatr Dent. 2001;23(1):37-43.
- Linnett V, Seow WK, Connor F, Shepherd R. Oral health of children with gastro-esophageal reflux disease: a controlled study. Aust Dent J. 2002;47(2):156-62.
- Bonuck K, Parikh S, Bassila M. Growth failure and sleep disordered breathing: a review of the literature. Int J Pediatr Otorhinolaryngol. 2006;70(5):769-78.
- Bonuck KA, Chervin RD, Cole TJ, Emond A, Henderson J, Xu L, et al. Prevalence and persistence of sleep disordered breathing symptoms in young children: a 6-year population-based cohort study. Sleep. 2011;34(7):875-84.
- Bonuck K, Rao T, Xu L. Pediatric sleep disorders and special educational need at 8 years: a population-based cohort study. Pediatrics. 2012;130(4):634-42.
- Bonuck K, Freeman K, Chervin RD, Xu L. Sleep-disordered breathing in a population-based cohort: behavioral outcomes at 4 and 7 years. Pediatrics. 2012;129(4):e857-65.
- G AA. Bruxism in children a warning sign for psychological problems. Jnl of Clinical Practise [Internet]. 2006; 72
No2
- Delgado Jimenez MC, Pujol Massaguer T. [Bruxism in children: a warning sign?]. Aten Primaria. 1996;17(2):172-3.
- Manfredini D, Serra-Negra J, Carboncini F, Lobbezoo F. Current Concepts of Bruxism. Int J Prosthodont. 2017;30(5):437–8.